by John Weeks, Publisher/Editor of The Integrator Blog News and Reports

The art of assisting a patient to make habit changes is less in having the right information than in the nature of the engagement. Who is the patient and what sort of communication does he or she favor? What are the practitioner’s favored means of engaging the patient? Is it a fit? These questions are front in center in a recent hard-copy issue of the American Hospital Association’s (AHA’s)
Trustee Magazine entitled “Patient Insights: Consumer segmentation helps health systems know their customers, delivery better services.” (A slightly
different online version is here.)
The article slices the concept of “patient segmentation” in a variety of ways relative to marketing, to cost-saving, and to fostering optimal engagement. For instance, explored is how Big Data can provide “a long list of details … that goes far beyond clinical and demographic information” about the delivery organization’s customers. Among these: number of prescriptions, level of education, number of children in the household – “just tons of information that deepens the level of knowledge that we have.” Big brother meets modern medicine.

The article’s interest to the integrative practitioner heightens with the “patient segmentation” used to inform the work of health coaches at Cincinnati’s
TriHealth Corporate Health. A vendor, c2b Solutions surveyed 9,000 US citizens on 400 questions. This led to a categorization into 5 separate segments into which individuals utilizing coaching for diabetes are categorized based on preferred communication and engagement styles. Coaches use both the knowledge of their own segment, and that of their patient to describe the work. The groups are:
- Direction takers (13 percent) – believe physicians are the most credible source of information; go to doctors at the first sign of problems; ignore advice only when it doesn’t fit their routines.
- Balance seekers (18 percent) – Dedicated to health and wellness but don’t pay as much attention to their doctors; prefer to come to their own conclusions; seek information via the internet or on their own.
- Willful endurers (27 percent) – Live for the here and now; resistant to changing habits; only visit doctors when it’s a must.
- Priority jugglers (18 percent) – Busy with other responsibilities; low investment in own health but invest in that of loved ones; put off health issues until they interfere with other responsibilities.
- Self-Achievers (24 percent) – The most proactive about their health; more likely than Balance Seekers to prioritize doctor’s advice; task oriented relative to check-ups/screenings; like measurable goals.
A short 12-question survey is used to place patients into one of these segments. The coaches also took it. In doing so, the coaches learned that they are “most comfortable” with patients in their own segment. Similarly, success with other segments “improves when [coaches] learn to speak in a different language … to communicate with individual who see the world differently than they do.” The segmentation work brought another big message to the delivery organization: the users of coaching services were disproportionately the more proactive Balance Seekers and Self Achievers.
Comment: In a funny little skit written by now osteopathic physician
Tom Harris, DO when he was in medical school 30
years ago, he has a character who is a physician-researcher say: “We all know how we are supposed to eat. It’s just getting people to do what they know is the right thing to do that is the problem.” The character goes on to describe his solution: “The actual grafting of vegetables onto the human body.” A slide pops onto the screen of a student with a zucchini for a forearm.
Even with as little information about the segments that is shared here, most integrative practitioners can pretty well categorize themselves, and quite likely - with a little probing - most of their patients. How many are you bludgeoning with just the wrong communication style? How might a different language with
this patient yield better results?
What would be particularly valuable would be to overlay on this set
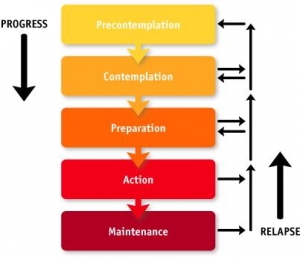
Prochaska’s readiness for categories: pre-contemplation, contemplation, preparation, action, maintenance, and termination. What better tools for a relationship-focused, communication-oriented, practitioner who recognizes that it is not depth biochemistry, or obscure pathways or genetic information but engaging patients in behavior change that is the core practitioner skill in health creation?
 years ago, he has a character who is a physician-researcher say: “We all know how we are supposed to eat. It’s just getting people to do what they know is the right thing to do that is the problem.” The character goes on to describe his solution: “The actual grafting of vegetables onto the human body.” A slide pops onto the screen of a student with a zucchini for a forearm. Even with as little information about the segments that is shared here, most integrative practitioners can pretty well categorize themselves, and quite likely - with a little probing - most of their patients. How many are you bludgeoning with just the wrong communication style? How might a different language with this patient yield better results? What would be particularly valuable would be to overlay on this set Prochaska’s readiness for categories: pre-contemplation, contemplation, preparation, action, maintenance, and termination. What better tools for a relationship-focused, communication-oriented, practitioner who recognizes that it is not depth biochemistry, or obscure pathways or genetic information but engaging patients in behavior change that is the core practitioner skill in health creation?
years ago, he has a character who is a physician-researcher say: “We all know how we are supposed to eat. It’s just getting people to do what they know is the right thing to do that is the problem.” The character goes on to describe his solution: “The actual grafting of vegetables onto the human body.” A slide pops onto the screen of a student with a zucchini for a forearm. Even with as little information about the segments that is shared here, most integrative practitioners can pretty well categorize themselves, and quite likely - with a little probing - most of their patients. How many are you bludgeoning with just the wrong communication style? How might a different language with this patient yield better results? What would be particularly valuable would be to overlay on this set Prochaska’s readiness for categories: pre-contemplation, contemplation, preparation, action, maintenance, and termination. What better tools for a relationship-focused, communication-oriented, practitioner who recognizes that it is not depth biochemistry, or obscure pathways or genetic information but engaging patients in behavior change that is the core practitioner skill in health creation?



















SHARE